What Is Azoospermia?
Azoospermia means the complete absence of any sperm in a man’s semen. It’s found in 5-10% of men who seek infertility treatment–so it’s a major cause of male infertility.
अशुक्राणुता: Azoospermia in Hindi
It may shock men when they find out they are infertile. There is still a common but incorrect belief that infertility is a woman’s problem. Therefore, when an andrologist or sexologist in Jaipur says there is a sperm problem, or azoospermia, or अशुक्राणुता, they are in disbelief
Being told that there is a sperm problem can affect a man’s sense of masculinity, sexuality, and potency.
But now with better sex education and awareness about sexual health, men in India now understand low testosterone problems, testes problems, erectile dysfunction, premature ejaculation, nightfall problems, ,and all other sexual problems as diseases, not weaknesses.
An emotional response to infertility is normal. Talking with a doctor or a sexual therapist or counsellor can help some men with their feelings about infertility.
There are three types of azoospermia:
- Pre-testicular azoospermia (non-obstructive): is caused by decreased sperm-producing hormone production.
- Testicular azoospermia (non-obstructive): is caused by any anomalies in the structure or operation of the testicles.
- Obstructive or post-testicular azoospermia: is caused by difficulties ejaculating as a result of some form of restriction in the reproductive system.
Strong Facts About Azoospermia in Men
- A man’s fertility generally relies on the quantity and quality of his sperm.
- A man suffering from azoospermia has a low number of sperm in ejaculation.
- With inferior quality sperm, it will be difficult, and sometimes impossible, for him to cause a pregnancy.
- We diagnosed male infertility only after testing both partners, and find reproductive problems in the male.
- About two-thirds of infertile men have a problem with making sperm in the testes.
- There are sperm transport problems in about one in every five infertile men
Understanding Sperm Anatomy
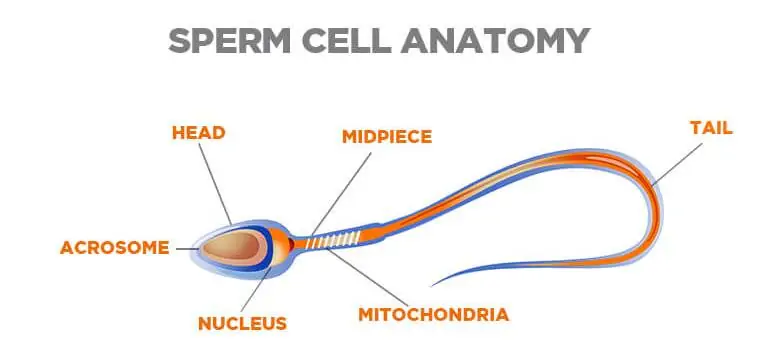
The testicles located outside the male body have two basic functions they produce: testosterone and sperm. The inside of the testicle has millions of hollow seminiferous tubules. Their walls comprise reproductive cells working for various stages of SPERM development.
Sperm production starts with a large round of immature cells the spermatogonia. This further divides and undergoes a multi-step 72-day maturation process.
Finally, becoming a sperm cell with a head and a tail.
Sperm, enter the epididymis where they are stored during ejaculation; The sperm travels through the vas deferens and prostate where they mix with seminal vesicle fluid to form semen. Normally, the seminiferous tubules continuously produce millions of sperm in the abdomen. We may find testicle sperm in small amounts in some of the tubules.
Symptoms of Azoospermia
If the number of sperm a man ejaculates is low or if the sperm is of poor quality, it will be difficult, and sometimes impossible, for him to cause a pregnancy.
When a couple cannot conceive after a repetitive try for a year, the testing for both partners’ reproductive problems can lead to male sperm problem Azoospermia.
There are no obvious symptoms of azoospermia as intercourse, erections and ejaculation will usually happen without difficulty. The quantity and appearance of the ejaculated semen generally appear normal to the naked eye.
It is only after Medical tests that Azoospermia in men is diagnosed with IASH.
Semen Analysis for Sperm Counts
The following are the normal semen analysis result, determined by World Health Organization (WHO):
| WHO Reference Range | |
| Total sperm count in the ejaculate | 39–928 million |
| Ejaculate Volume | 1.5–7.6 mL |
| Sperm Concentration | 15–259 million per mL |
| Total Motility | 40–81% |
| Progressive Motility | 32–75% |
| Sperm morphology | 4–48% |
A semen analysis to check the number, shape and movement of sperm in the ejaculate. We may also do blood tests to check the levels of hormones that control sperm production or for genetic testing. For some, we prescribe testicular biopsies or testicular ultrasounds.
Sperm analysis done in a lab that has the capability of sperm freezing immediately is best. When done at regular labs there are high chances of missing sperm and getting misleading reports. This is valuable biological material that cannot be used as waste. Hence sperm analysis at IASH is at a lab that has a sperm freezing capability.
Causes of Azoospermia
Problems that affect either sperm production or sperm transport usually cause male Azoospermia. Through medical testing, the doctor may be able to find the cause of the problem.
Moving further, we generally divide the causes of azoospermia into obstructive, and non-obstructive.
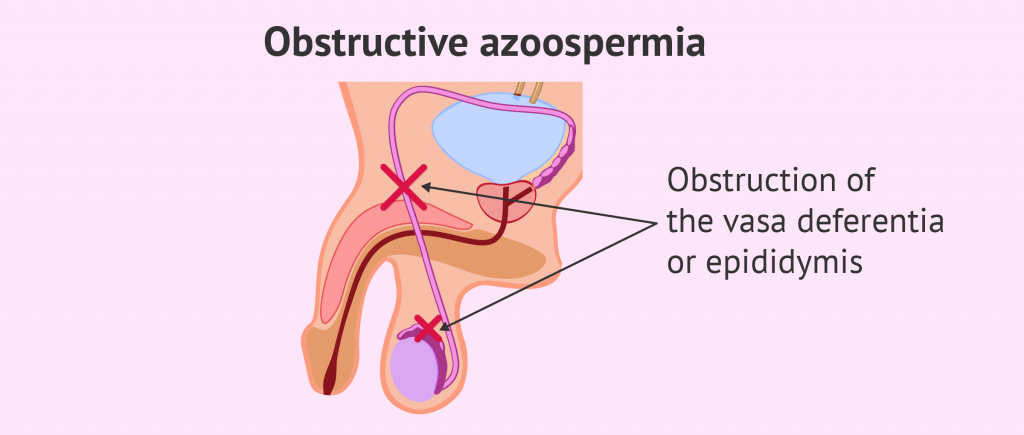
Obstructive Azoospermia
It is when sperm is blocked from exiting the testicles. Because of an injury, infection, prior surgery, or a genetic defect, the sperm cannot transit from testicles. The other causes of obstructive azoospermia are:
- Infections
- Prostate-related problems
- Absence of vas deferens
- Vasectomy
There are sperm transport problems in about one in every five infertile men, including men who have had a vasectomy but now wish to have more children. Blockages (often referred to as obstructions) in the tubes leading sperm away from the testes to the penis can cause a complete lack of sperm in the ejaculated semen.
Non-Obstructive Azoospermia
About two-thirds of infertile men have a problem with making sperm in the testes. Either testis produces low numbers of sperm /or the sperm that are made do not work properly. The other causes of non-obstructive azoospermia are:
- Chromosomal or genetic causes
- Undescended testes (failure of the testes to descend at birth)
- Infections
- Torsion (twisting of the testis in the scrotum)
- Varicocele (varicose veins of the testes)
- Medicines and chemicals
- Other Ejaculation Problems like Retrograde Ejaculation, Epididymis
- Radiation damage
- Unknown cause
Some changes to chromosomes or gene mutations cause abnormal sperm production or blockages to sperm flow that lead to male infertility. The most common genetic causes of infertility are chromosomal conditions that affect sperm production. These include:
- Klinefelter’s syndrome
- Y chromosome deletions
- other genetic problems, such as Down syndrome.
Oligospermia

Now, sometimes when there is no sperm in a man’s ejaculate, it’s because it’s being produced at very low levels, and there is still some sperm in the man’s testes. This is a case of severe oligospermia, and while it’s still very serious, sperm retrieval and assisted reproductive technology could still make pregnancy a possibility.
Azoospermia Treatment
Azoospermia or the condition of no sperm in the ejaculate primary cause is either by a blockage in the reproductive tract or a deficiency in sperm production.
IASH provides sperm harvesting techniques to address these different scenarios based on the patient’s condition. When there is a blockage, we can remove sperm from the epididymis via a procedure called microsurgical epididymal sperm aspiration or MESA.
There are a number of ways to get sperm from the epididymis but MESA treatment at IASH is a relatively painless and minimally invasive procedure performed under local anaesthesia.
If you have obstructive azoospermia, there are minimally invasive surgeries available to correct many of the causes.
Treating non-obstructive azoospermia can be more difficult depending on the cause. In cases where lifestyle factors are an issue, such as medication usage, or hormonal imbalance, treatment can be as simple as changing the medications or addressing those hormone problems.
Ayurvedic Medicine for Azoospermia

Dr Chirag Bhandari, the Best Sexologist in Jaipur, prescribes Ayurveda medicines that help to improve sperm count by enhancing the quality of semen. The medicines he prescribes are a mixed chemical composition of natural herbs like Ashwagandha, Shankhpushpi, fenugreek seeds, Gokharu, Safed Musli, and Konch Beej.
His patients have reviews about improving the quality of their semen in terms of its thickness, sperm count, semen volume etc after consuming it regularly.
Daily dosage of Zinc supplements can also help to improve sperm count and avoid azoospermia in men.
However, in cases of genetic mutation or other things that are not easily treatable, IVF with a sperm donor may be your best option. At the present time, men with genetic problems can father children naturally, with IVF, ICSI or other forms of assisted reproduction offering the best chance for these men to have biological children.
Tips To prevent Azoospermia
If the azoospermia is not genetic then you can try avoiding the below things to prevent azoospermia:
- Keep radiation exposure to a minimum.
- Stay away from activities and sports that may harm your reproductive organs.
- Discuss the benefits and drawbacks of medications that could affect sperm production with your doctor.
- Avoid using saunas or steam rooms or engaging in other activities that could subject your testicles to extreme heat.
- It is best to avoid cigarette smoking, excess alcohol, sexually transmitted diseases, heat stress from tight-fitting underwear, and anabolic steroids (taken for body building or sporting purposes) as these factors can be harmful to the production of sperm.
The Takeaway
It can be frightening to receive an azoospermia diagnosis or to hear “no sperm count.” Breathe deeply – just because you have this issue doesn’t mean you can’t have biological children.
It’s critical to first comprehend the problem’s root cause. At IASH Jaipur we suggest several treatments to remove the blockage after discussing and addressing the problem. Otherwise, treatments like IVF could be able to assist you and your partner conceive.
Frequently Asked Questions
Q1. Can Azoospermia be cured?
Ans. Fertility can perhaps be restored if hormonal issues and obstructive causes of azoospermia are treated. Even if testicular problems are to blame, viable sperm can still be obtained and used in assisted reproductive methods.
Q2. Can a man with no sperm count have a baby?
Ans. The answer is yes. A man with no sperm count can have a baby with the art methods like IVF, ICSI etc.
Q3. Why Would a Man have no sperm?
Ans. Low or no sperm production may result from reproductive system damage. A blockage (obstruction) within the tubes the sperm pass through is present in about 4 out of every 10 men who have azoospermia, or absolute lack of sperm. A blockage may be brought on by an illness or a congenital abnormality.

